Pneumococcal Disease
What is pneumococcal disease?
Streptococcus pneumoniae (‘pneumococcus’) is the most common bacterial cause of community-acquired pneumonia and a common cause of bacteraemia and meningitis in children and adults. There are over 90 types of S. pneumoniae known (these are called serotypes). Disease caused by any S. pneumoniae serotypes is called pneumococcal disease.
What diseases does pneumococcus cause?
The most common types of infections caused by S. pneumoniae include:
- Middle ear infections (acute otitis media), particularly common in children
- Pneumonia
- Bacteraemia (blood stream infection)
- Sinus infections and
- Meningitis
How common is pneumococcal disease?
Pneumococcal infection is a leading cause of death worldwide. Mortality is highest in patients who develop bacteraemia or meningitis. Pneumococcal pneumonia is estimated to affect 0.1% of the population every year. Pneumococcal pneumonia is more common in smokers, heavy drinkers and those who live in over-crowded sleeping quarters.
Who is most at risk of pneumococcal disease?
Individuals most at risk of pneumococcal infections are usually the very young or the elderly. Those with the following conditions are particularly vulnerable and the National Immunisation Advisory Committee (NIAC) recommends pneumococcal vaccines to the following individuals:
- Persons 65 years of age or older
- Children under 5 years of age
- Asplenia (no spleen) or severe dysfunction of the spleen, including surgical splenectomy
- Chronic renal disease or nephrotic syndrome
- Chronic heart, lung or liver disease, including cirrhosis
- Diabetes mellitus
- Sickle cell disease
- Weakened immunity (due to disease or treatment)
- Complement deficiency
- Patients with CSF leaks, either congenital or complicating skull fracture or neurosurgery
- Individuals with cochlear implants
- Smokers and alcoholics
- Individuals with occupational exposure to metal fumes (i.e. welders)
How do people get infected?
Transmission is from person to person, usually through respiratory droplet spread, but may be by direct oral contact or indirectly through articles contaminated with respiratory discharges. The S. pneumoniae bacteria are spread through contact between persons who are ill or who carry the bacteria in their throat (often without being ill). The incubation period (time between exposure to the bacteria and becoming ill) varies by type of infection and can be as short as one to three days.
How is pneumococcal disease treated?
Pneumococcal disease is treated with antibiotics. In recent years many pneumococci have become resistant to some of the antibiotics used to treat pneumococcal infections; in 2018 21 % of samples tested by the National Pneumococcal Reference Laboratory were non-susceptible to penicillin an increase since 2014 when 17% of penicillin samples were resistant.
How is pneumococcal disease prevented?
The most common strains S. pneumonia (serotypes) can be prevented by vaccination. Some strains, not covered by the vaccines will occur despite vaccination. Vaccination is recommended for those most at risk of disease (identified in previous sections and in table below).
Pneumococcal vaccines
There are two different types of pneumococcal vaccines:
- Pneumococcal Polysaccharide Vaccine (PPV23). This incorporates 23 of the most common capsular types*, which account for up to 90% of all serious pneumococcal infections. It is only suitable for use in those ≥2 years of age; an adequate antibody response does not develop in those under 2 years of age.
- Pneumococcal Conjugate Vaccines (PCV 7, 10 and 13) contain polysaccharide antigens from 7, 10 or 13 serotypes conjugated to a protein (see below for details on which serotypes are contained in each vaccine). These vaccines provide protection against 75-90% of serotypes causing invasive disease, including a significant number of penicillin-resistant strains. The number of doses required for optimum immune response depends on the age at which the vaccine is given.
Recent changes in vaccines used in childhood immunisation programme
In Ireland PCV7 was recommended for at risk children in 2002. In September 2008 it was recommended for all infants, along with a catch up programme for all children under 2 years of age. In December 2010 PCV13 vaccine replaced PCV7 in the Irish childhood immunisation programme. PCV13 includes antigens from the seven serotypes contained in PCV7 plus six additional serotypes which cause IPD.
The introduction of PCV vaccine resulted in a dramatic decline in incidence of invasive pneumococcal disease in children < 5 years of age (94% decline) in 2018. See quarterly reports on Invasive Pneumococcal Disease in Ireland for more information on impact.
In 2018, NIAC recommended the use of PCV vaccination for children and adults at medium and high risk of invasive pneumococcal disease (see table). Updated information can be found in most recent NIAC guidance.
Clinical risk groups who require pneumococcal vaccination:
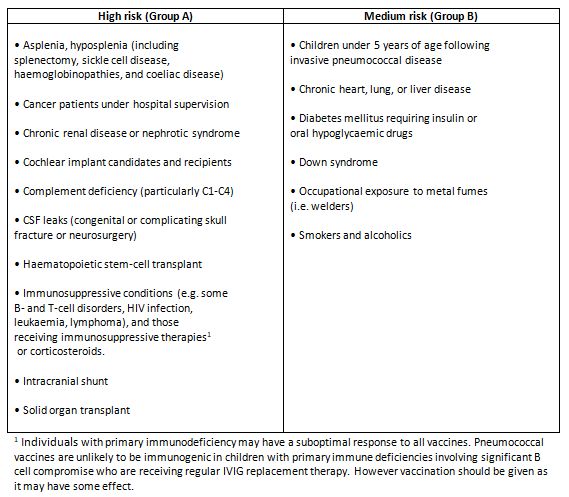
What serotypes are covered by the different vaccines?
The following serotypes are contained in pneumococcal vaccines:
PCV7: 4, 6B, 9V, 14, 18C, 19F, 23F
PCV10: 1, 4, 5, 6B, 7F, 9V, 14 18C, 19F, 23F
PCV13: 1, 3, 4, 5, 6A, 6B, 7F, 9V, 14, 18C, 19A, 19F, 23F
*PPV23: 1, 2, 3, 4, 5, 6B, 7F, 8, 9N, 9V, 10A, 11A, 12F, 14, 15B, 17F, 18C, 19A, 19F, 20, 22F, 23F, 33F
What vaccine and how many doses should babies get to protect against pneumococcal disease?
Two doses of the pneumococcal conjugate vaccine are recommended in infancy (< 1 year of age). The doses are given at the ages of 2, 6 with a booster at 13 months of age. Due to the introduction of Men B vaccine in to routine immunisation the third dose of PCV 13 was shifted from 12 months of age to 13 months of age in December 2016 for children born on or after 1st October 2016. It is important that children receive all the doses at the right time to protect them from pneumococcal disease. See the Pneumococcal Chapter of the NIAC guidelines for more information, available here.
Do some children need additional protection against pneumococcal disease?
Some children are at particularly high risk of pneumococcal infection (see conditions listed above) and may be recommended either additional doses of either the PCV13 and/or the polysaccharide vaccine (PPV23) to provide broader protection. See the Pneumococcal Chapter of the NIAC guidelines for more information, available here.
Are booster doses of the PPV23 recommended?
The Pneumococcal Polysaccharide Vaccine (PPV23) is recommended for individuals at increased risk of pneumococcal disease (as outlined above);
Booster doses are not recommended for immunocompetent people aged <65 years. The administration of a first dose of PPV23 may blunt the immune response to subsequent doses of both PPV23 and PCV13, such that antibody levels following a second vaccination, and possibly the magnitude of clinical protection, may be lower than following a first vaccination. For individuals whose antibody levels are likely to decline more rapidly, (e.g. those with no spleen, with splenic dysfunction, and immunosuppression) one booster should be given 5 years after the first dose.
Adults 65 years or older should receive a second dose of PPV23 if they received vaccine more than 5 years before and were less than 65 years of age at the time of the first dose.
Those who received one dose of PPV23 at age 65 or older do not require any further dose regardless of immune status.
For more information on pneumococcal vaccines please see the Immunisation Guidelines 2018
For details on the epidemiology of pneumococcal disease in Ireland click here.
Last updated: 11th December 2019


