Bacterial Meningitis/Meningococcal Disease
What is meningitis?
Meningitis is an inflammation of the meninges, which is the name given to the covering layer of the brain and spinal cord.
What is septicaemia?
Septicaemia is a form of blood poisoning caused by the same organisms that can cause meningitis.
What causes bacterial meningitis and/or septicaemia?
Most cases are caused by a few specific bacteria, including Neisseria meningitidis (meningococcus), Streptococcus pneumoniae (pneumococcus), and Haemophilus influenzae. TB meningitis is a rare form of meningitis caused by the bacteria that causes tuberculosis (TB). Newborn infants are also susceptible to certain other types of bacterial meningitis including those caused by Escherichia coli, Listeria monocytogenes and group B streptococcus.
What are the signs and symptoms of meningitis and septicaemia?
Visit the HSE Meningitis and septicaemia - symptoms website to see common signs & symptoms of meningitis and septicaemia in babies & toddlers, children & teens and adults. Some of the signs and symptoms are described below.
Signs and symptoms of meningitis and septicaemia
- Meningitis and septicaemia often happen together. Symptoms can appear in any order, some may not appear at all.
- Early symptoms can include fever, headache, vomiting, diarrhoea, muscle pain, stomach cramps, fever with cold hands and feet.
- Think about meningitis and septicaemia if you or your child has any of these symptoms:
- a high temperature of 38 degrees Celsius or above
- a rash or spots (this may be harder to see on brown or black skin)
- feeling and being sick
- headache
- a stiff neck
- aches or pains - for example, stomach, joint or muscle pain
- breathing fast
- bothered by bright light
- cold hands and feet or pale, mottled skin
- fits (seizures)
- Other symptoms include:
- confusion
- drowsiness
- hard to wake them up
- irritability
- lack of energy
- Babies may also:
- refuse feeds or feed less
- be agitated
- not want to be picked up
- have a bulging soft spot on their head (fontanelle)
- have an unusual high-pitched cry
- have a stiff body
- be floppy or unresponsive
Figure 1 and Figure 2 show examples of the rash due to septicaemia.
Figure 3 shows what is called the tumbler test. If you press a glass tumbler against this rash, it will not disappear. You will still be able to see it through the glass.
Figure 1. Figure 2. Figure 3.
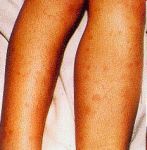
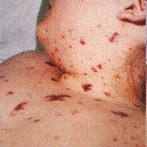
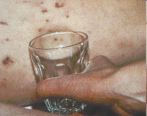
(Figures 1,2 and 3 were kindly provided by the Meningitis Research Foundation)
DO NOT WAIT FOR A RASH. If someone is ill and getting worse, get medical help immediately. Call 112 or 999 for an ambulance immediately or go to your nearest emergency department (ED) or ED for children if you think that you or your child is seriously ill.
Can bacterial meningitis and septicaemia be treated?
All types of bacterial meningitis and septicaemia can be treated with antibiotics.
How many cases of bacterial meningitis are seen each year in Ireland?
Information on the number of bacterial meningitis cases notified in Ireland is available on the HPSC Notifiable Diseases Hub.
Invasive Meningococcal disease
What is invasive meningococcal disease?
Invasive meningococcal disease is the most common form of bacterial meningitis in Ireland, causing up to 90% of the cases. This disease may present as meningitis, septicaemia (blood poisoning) or both.
What causes invasive meningococcal disease?
Neisseria meningitidis is the name of the bacteria that is responsible. There are several different types of Neisseria meningitidis, these include groups A, B, C, W135 and Y. Group B is the most common form seen in Ireland. Since the vaccine for Meningococcal Group C disease was introduced in October 2000, there has been a dramatic decline in the number of bacterial meningitis cases occurring each year.
How do you get invasive meningococcal disease?
The infection is usually spread by people who carry these bacteria in their nose or throat but are not ill themselves. It is spread by respiratory droplets, which are caused by coughing, sneezing and mouth kissing. Less commonly, the infection can be spread by someone with meningitis. Depending on the age group, up to 1 in 10 people may carry these bacteria.
Who is most at risk?
Invasive meningococcal disease may occur at any age but is most common in infancy and early childhood with an additional smaller peak of disease activity in adolescents and young adults. In temperate climates such as Ireland the infection typically shows a seasonal variation with most cases occurring in winter and early spring.
Can invasive meningococcal disease be treated?
The answer is yes. The earlier the diagnosis, the earlier treatment with antibiotics can begin and therefore the greater chance that the person will make a full recovery. Early diagnosis is the key so if you suspect that someone may have meningitis or septicaemia seek medical attention immediately.
Is there a vaccine available for invasive meningococcal disease?
Yes, there are vaccines available for meningitis. When talking about vaccines it is important to remember that there are several different types of Neisseria meningitidis bacteria, including groups A, B, C, W135 and Y with groups B being the most common in Ireland.
Vaccines to protect against invasive meningococcal disease
Meningococcal B vaccine
The meningitis B vaccine offers protection against meningococcal group B bacteria. These bacteria are a common cause of meningitis in young children. The vaccine is recommended for babies aged 2 months. This is followed by a second dose at 4 months, and a third one at 12 months.
Meningococcal C (Men C) vaccine
The Meningococcal C vaccine offers protection against meningococcal group C bacteria. This bacterial infection can cause meningitis and septicaemia. The number of cases of meningococcal disease due to group C bacteria has fallen dramatically since the vaccine was introduced. If your child was born before 1 October 2024, they will get the vaccine at 6 months. A MenC booster is given at 13 months of age at the same time as the Hib vaccine. If your child was born on or after 1 October 2024, they will only need 1 vaccine in early childhood, at 13 months of age.
Meningococcal ACWY vaccine
The MenACWY (meningococcal ACWY) vaccine protects against 4 types of bacteria that can cause meningitis. These are meningococcal groups A, C, W and Y. Your child will be offered this vaccine in the first year of secondary school.
Other types of bacterial meningitis
Apart from invasive meningococcal disease (caused by Neisseria meningitidis) the next most common form of bacterial meningitis is pneumococcal meningitis (caused by Streptococcus pneumoniae). Hib meningitis (caused by Haemophilus influenzae type b) was a major cause of meningitis in infants previously but has now been almost entirely eliminated following the introduction of Hib vaccine as part of the Primary Childhood Immunisation Programme in 1992.
TB meningitis is a rare form of meningitis caused by the bacteria that causes tuberculosis (TB).
Newborn infants are also susceptible to certain other types of bacterial meningitis including those caused by Escherichia coli, Listeria monocytogenes and group B streptococcus.
All types of bacterial meningitis are treated with antibiotics.
Vaccines for other forms of bacterial meningitis
6-in-1 vaccine
The 6-in-1 vaccine is also known as the DTaP/IPV/Hib/Hep B vaccine. It protects against 6 types of bacteria, including Haemophilus influenzae type b (Hib) which is a type of bacteria that can cause meningitis. 6-in-1 vaccine is given to babies at: 2 months, 4 months and 6 months of age. Babies receive a 4th dose of Hib vaccine aged 13 months, as part of a MenC/Hib vaccine if born before October 1st 2024 and as part of a 4th dose of 6-in-1 vaccine if born on or after 1st October 2024.
Pneumococcal vaccine
The pneumococcal vaccine protects against serious infections, including meningitis, caused by Streptococcus pneumoniae bacteria. Babies receive the pneumococcal vaccine (PCV13) as 3 separate injections. These are at 2, 6 and 12 months of age for babies born before October 1st 2024 and at 2, 6 and 13 months of age for babies born on or after October 1st 2024.
A second type of pneumococcal vaccine (PPV23) is given to older adults. A single dose of PPV23 is recommended for all adults aged 65 years and older.
For further information about vaccines, please visit the HSE National Immunisation Office website at immunisation.ie
Last updated: 29 January 2026


